The Johns Hopkins ACG System is the world’s leading population health analytics software. The system continues to evolve, providing ever-more refined tools used in the US and across the globe for over 30 years, from commercial health plans and governments to health systems and large employers. The beauty of the ACG System is its ability to combine data from an array of sources to reveal powerful insights that go beyond just medical records. By identifying risk and tracking patients over time, the ACG System can help you plan ahead and reduce health care costs—especially valuable to risk-bearing health systems and provider organizations. Most importantly, the ACG System allows you to be proactive rather than reactive when it comes to your population’s unique health care needs. The system helps you combine a population-level perspective with patient-level behaviors and conditions. And because the system is incredibly flexible and responsive to new information, you can rest assured that no matter what comes next, the ACG System will continuously adapt to your health care management needs.
What is an “ACG®” or “Adjusted Clinical Group®”?
Based on the premise that clustering of morbidity is a better predictor of health care services resource use than the presence of specific diseases or disease hierarchies, the ACG System provides a multi-morbidity framework that is clinically logical, informative of future health care resources, easy to use and applicable to both financial and clinical managers.
What Sets the ACG System Apart?

Allows for Transparency

Relevant for Any Population

Clinical Relevance

Global Reach

Person-Centered Approach

Predictive Models

Reveals Performance Drivers

University Backing
Streamline Care Management
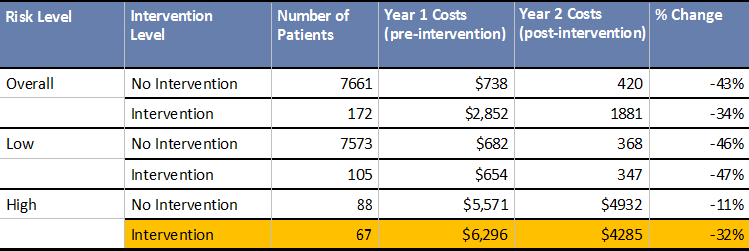
With the ACG System you can identify up to 25% more individuals for care management before they become high utilizers. Optimize your case management and disease management programs by targeting individuals, assessing patient risk and identifying those who would benefit the most.
Improve Outcomes with Care Coordination
Reduce Health Care Cost and Improve Patient Health Outcomes
Coordination exerts an important impact on both the efficiency and effectiveness of care. Patients most in need of highly coordinated care include those with multiple chronic medical conditions, concurrent care from several health professionals or many medications and patients undergoing extensive diagnostic workups or transitions from one setting of care to another.
The ACG System Utilization Profile Report includes many concepts to evaluate population health, including concurrent and prospective risk, risk factors, utilization, disease prevalence, pharmacy adherence and care coordination risk.
Assess Physician Performance
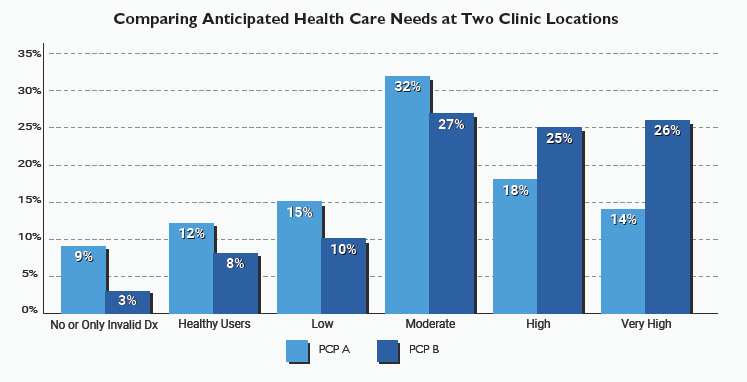
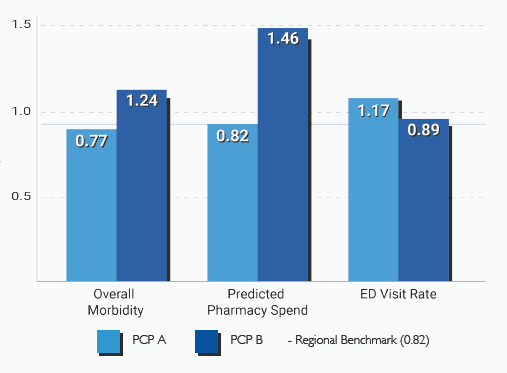
The ACG System performance analysis takes into account the health of the particular population served by a specific clinician or set of clinicians, addressing important differences in casemix and the often stated concern that “my patients are sicker.” Because a disease-based focus may miss important implications of related co-morbidities, we provide a holistic view of the patient rather than the management of specific diseases or episodes.
Allocate Resources Appropriately
The ACG System is widely used by health plans and health systems for risk adjustment, setting capitation rates, insurance premiums and for appropriately distributing health care resources within large health systems. The ACG System helps health care providers, payers and governments worldwide ensure that resources appropriately target populations in greatest need.
Gain Prompt Insights from Pharmacy Data
The ACG System can use pharmacy claims data as an input to supplement diagnosis information from claims data. The inclusion of pharmacy data can enhance the performance of the predictive models within the ACG System but can also be used to create several specific, pharmacy-related outputs. These outputs include:
- A count of all unique medication types to highlight polypharmacy
- Potential gaps in the provision of medication for high-risk patients and those with chronic conditions
- Identification of patients who may not be receiving appropriate treatment of their condition
- Identification of patients who are receiving treatment for a condition that has not been recorded in their EMR